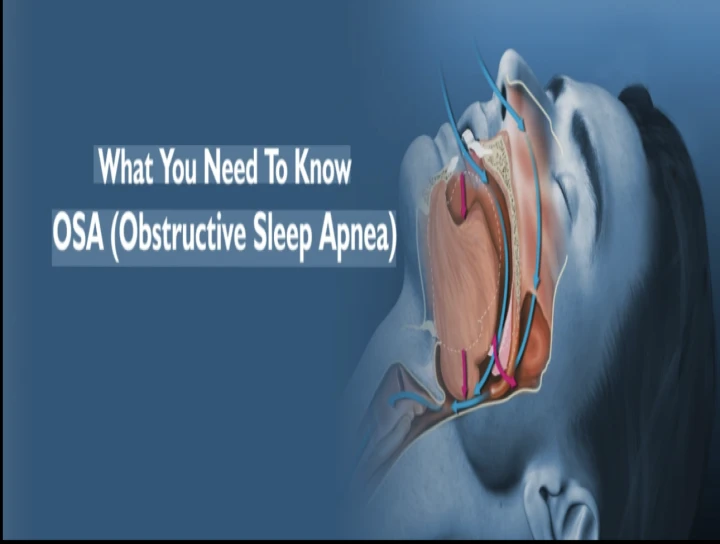
Obstructive Sleep Apnea
Obstructive sleep apnea syndrome is a serious condition that afflicts a substantial number of individuals. It is characterized by disruption of normal sleep architecture by complete or partial obstruction of respiratory airflow. Airflow obstruction results in a reduction of blood oxygen saturation known ashypoxemia. It produces arousal in an attempt to reopen the airway. These recurring arousals disrupt sleep architecture, which diminishes the quality of sleep. This cycle results in excessive daytime somnolence, which is one of the hallmark features of this disease condition. If untreated, obstructive sleep apnea syndrome greatly shortens the expected life span from many associated comorbidities, such as increased rates of cardiovascular and pulmonary disease and obesity related diabetes mellitus.
Obstructive sleep disordered breathing is a relatively common medical problem. It consists of a spectrum ranging from apnea to hypopnea. Obstructive apnea refers to the temporary cessation of airflow during sleep for 10 seconds or more despite continuing ventilatory effort, whereas hypopnea means reduction of30% to 50% in airflow for 10 secs or more. Obstructive sleep apnea(OSA) the most widely known disorder in the category affects 2% to 4% of middle agedadults.
PATHOGENESIS-The definitive event in OSA is occlusion of the upper airway usually at the level of the oropharynx. The resulting apnea leads to progressive asphyxia until there is a brief arousal from sleep, whereupon airway patency is restored and airflow resumes. The patient then returns to sleep, and the sequence of events is repeated, often up to 400 to 500 times per night, resulting in marked fragmentation of sleep.
The immediate factor leading to collapse of the upper airway in OSA is the generation of a critical sub atmospheric pressure during inspiration that exceeds the ability of the airway dilator and abductor muscles to maintain airway stability. Sleep plays a permissive but crucial role by reducing the activity of the muscles to sub atmospheric airway pressures. Alcohol is frequently an important cofactor because of its selective depressant influence on the upper airway muscles and on the arousal response that terminates each apnea. In most patients the patency of the airway is also compromised structurally and therefore predisposed tooth occlusion. Obesity frequently contributes to the reduction in size of upper airways, either by increasing fat deposition in the soft tissues of the pharynx or by compressing the pharynx by superficial fat masses in the neck. Snoring, a high frequency vibration of the palatal and pharyngeal soft tissues that results from the decrease in size of the upper airway lumen, may aggravate the narrowing by producing edema of the soft tissues. More sophisticated studies demonstrate a high airway compliance i.e. the airway is “floppy” and therefore prone to collapse.
In some patients, a high upstream (i.e. nasal) resistance predisposes to collapse Of the upper airway by increasing the sub atmospheric pressure generated in the pharynx during inspiration as the strength of9 diaphragmatic contraction is increased to overcome airflow resistance in the nose.
ETIOLOGY
The respiratory disturbances associated with sleep vary by degree
Apnea : the cessation of airflow at the nose and mouth for 10 seconds or longer.
Hypopnea : a reduction in airflow at the nose and mouth2. In addition, apneas or hypopneas may vary by mechanism.
1. Obstructive: The resistance of the upper airway increases.
2. Central: Respiratory effort is reduced or ceases.
3. Mixed: a period of central apnea followed by several obstructed breaths. These have the same clinical implications as purely obstructive events. Following generally accepted usage, the asymptomatic disorder is defined as sleep apnea (central or obstructive); sleep apnea syndrome (central orobstructive) is diagnosed when symptoms occur.
In addition, the upper airway resistance syndrome has recently been described and is regarded as a variant of obstructive sleep apnea syndrome. In this disorder, upper airway caliber is diminished during sleep, and respiratory effort increases to maintain normal airflow. The increased effort results in recurrent arousal from sleep (termed respiratory effort-related arousal) and produces daytime sleepiness in a manner similar to obstructive sleep apnea syndrome.
4. Central sleep apnea syndrome is a relatively uncommon entity most frequently associated with congestive heart failure or central nervous system disease.
Several mechanisms may contribute to-
a. reduced upper airway caliber, caused by the following:
i. Obesity (collections of adipose tissue have been demonstrated adjacent to the airway)
ii. Adenotonsillar hypertrophy (usually in children)
iii. Mandibular deficiency (e.g., micrognathia or retrognathia)
iv. Macroglossia (frequently associated with hypothyroidism)
v. Upper airway tumors (rare)
b. Excessive pressure across the collapsible segment, most frequently attributed to nasal obstruction. Activity of the muscles of the upper airway are insufficient to maintain patency. Electromyographic studies have demonstrated reduced electrical activity of these muscles during apneas, consistent with a defect in respiratory control. The exact nature of this respiratory controlling stability is not known.
PROSTHETIC MANAGEMENTINTRAORAL APPLIANCES
An oral appliance was considered as treatment for mandibular deficiency and upper airway obstruction as early as 1902.
With the recent interest in sleep apnea, oral appliances of various designs have been proposed and studied, and are used increasingly to treat snoring and sleep apnea. The purpose of this review is to evaluate evidence regarding the effectiveness of these devices. The term “Oral appliance” is used as a generic term for devices inserted into the mouth in order to modify the position of the mandible, the tongue , and the structures in the upper airway for the purpose of relieving snoring or sleep apnea. Although many of these devices attach to the teeth and use conventional dental technology, we use the more general term to include devices that are used intraorally but are not necessarily retained directly by the teeth. Multiple devices have been developed for the treatment of obstructive sleep apnea. There are basically two major types – those that advance the tongue and those that advance the mandible.
The tongue retaining device (TRD) was one of the first appliances developed. It is a custom made appliance with an anterior bulb. It fits over both the upper and lower dental arches. The tongue is held in a forward position in the anterior compartment by suction. A flange fits between lips and the teeth and holds the device and the tongue forward in the oral cavity. Several mandibular positioning devices have been studied. Although most require dental impressions, bite registration and fabrication by a dental laboratory, devices are now available with a thermal labile material.
RATIONALE FOR THE USE OF MANDIBULAR ADVANCEMENTSPLINTS (MAS)
The role of dental appliances in the management of upper airway obstruction was recognised as early as 1902. A number of cephalometric studies, based on the use of a MAS, have shown an increase in upper airway dimensions in awake subjects. The limitations of a 2-dimensional view demonstrating antero-posterior changes, in evaluating airway responses to MAS must not be underestimated. However, only limited data are available on the effects of MAS in the transverse plane. Computerised tomography has been used to demonstrate that not only an increase in the airway space but also a change in shape accompanies the use of an oral appliances. More recently, Ryan et al, using video fluoroscopy, described increases in cross-sectional area of the upper airway, particularly in the velopharynx, when a MAS was worn. Gale et al. described the use of low dose computerised tomography to visualise 3-dimensional changes in the airway following the insertion of an anterior mandibular positioning appliance (AMPA).The authors demonstrated an increase in minimum pharyngeal cross-sectional area accompanied the use of an AMPA but were unable to link this to patient response to improvement in symptoms, in light of the wide but unpredictable changes observed. Despite the considerable variation in MAS design, the clinical effects appear remarkably consistent , OSA improves in the majority of subjects. Based on the findings of a review of twenty-one publications, undertaken by the American Sleep Disorders Association, the mean apnoea hypopnoea index (AHI) appeared to reduce from 47 to 19. However, whilst the authors completed a comprehensive review of all available published data on the use of intra-oral appliances for the management of OSA, the review has several limitations: It consisted entirely of case series, with relatively small sample size . Randomised controlled studies were lacking Descriptions of the patients, their selection criteria and the study methods used were varied and incomplete. More recently, a small number of well designed prospective randomised studies have been described in the literature.
Two of these compared the use of a mandibular advancement splint with nasal CPAP 118,119 and concluded that the MAS achieved substantial success (45% reduction in AHI score), but were less effective than n-CPAP (70% reduction in AHI score). Although the compliance rate was similar, the MAS was strongly preferred over n-CPAP. Bloch et al 120compared the effects of two different MAS designs with no treatment intervention and found the AHI reduced from 22.6 (no treatment intervention) to 8.7 (two-piece appliance) and 7.9 (single-piece appliance). Tegelberg et al, 121 in a prospective randomised study compared the effects of surgery of the oropharynx with MAS therapy. The authors report that 95% of the patients who completed the study reduced their AHI by 50% or more. This compared favourably with the results of the surgical arm of their study.
MECHANISM OF ACTION HOW DO ORAL APPLIANCES WORK?
The goal of any oral appliance for the treatment of snoring or OSA is to enlarge the airway or at least reduce the collapsibility between the soft palate and the posterior pharyngeal wall. The 3 general types of devices are discussed below.
Types of Devices Mandibular positioning (advancing) devices : By attaching to one or both dental arches, the intent is to advance or downwardly rotate the mandible. Most devices require a specialized, individualized design to properly fit the device to the individual. A qualified dental laboratory takes the impressions and fabricates the custom-made device. These are the most popular and useful devices. One manufacturer makes a device of a thermo labile material that is designed to be molded and fitted in the office. Tongue-retaining devices: The aim of this design is to secure the tongue by negative pressure into a soft plastic bulb, thereby forcibly holding the tongue anteriorly while sleeping. Although this is an attractive concept, for obvious reasons of comfort and compliance few patients like such devices.
Palatal lifting devices: These devices have not demonstrated efficacy in reducing either snoring or OSA and are not recommended by the Sleep Disorders Dental Society.
Snore Guard is a boil and bite appliance that is easy to fit and adjust directly on the patient and appears to be well tolerated. The mandible is positioned 3 mm behind maximum protrusion with a 7 mm opening. The appliance covers the anterior teeth only and is lined with a soft polyvinyl for patient comfort. The Snore Guard has received FDA market clearance only for the treatment of snoring. Schmidt-Nowara found that after 7 months of use in 68 patients, 75%of the individuals were using the appliance regularly. Snoring was decreased in all but one subject and eliminated in 29. In 20 OSA subjects, polysomnography revealed a mean RDI decrease from 47.4 to 19.7. In addition, oxygenation and sleep disturbance were improved. Ferguson et al compared the efficacy, side effects, patient compliance, and preference between 4 months of Snore Guard and nCPAP therapies in a randomized, prospective, crossover study in patients with
mild-to-moderate OSA. The RDI was lower with nCPAP than with the oral appliances. Some 48%of the patients who used the Snore Guard were treatment successes (reduction of RDI to < 10 per hour and relief of symptoms), 24% were compliance failures, and 28% were treatment failures. Four people refused to use nCPAP after using the Snore Guard. Some 62% of the patients who used nCPAP were overall treatment successes, 38% were compliance failures, and there were no treatment failures. Side effects were more common and the patients were less satisfied with nCPAP. Seven patients were treatment successes with both treatments; six of these patients preferred Snore Guard and one preferred nCPAP as a long-term treatment. The Snore Guard is an effective treatment in some patients with mild-to-moderate OSA and is associated with fewer side effects and greater patient satisfaction than nCPAP. The advantages of the Snore Guard are its relatively low cost and reduced clinical time required by the dentist; however, it is non adjust-able, it may apply excessive pressure to the lower anterior teeth in some patients, and retention problems may develop over time.
TheraSnoreThe adjustable - Therasnore is an adjustable boil and bite appliance available on the market and has received FDA market approval only for the treatment of snoring. The appliance consists of upper and lower trays that snap together by means of four locking mechanisms. Both trays are made of a thermoplastic material surrounded by a harder polycarbonate frame.
The TheraSnore can be adjusted forward or backward in 1.5-mm increments. The upper tray is designed to fit over the maxilla and the lower tray prevents the tongue and jaw from dropping backward during sleep. The appliance is fitted to the patient's centric occlusion and the mandible can be advanced by using the position indicators on the appliance. In 13 subjects with OSA, Schmidt-Nowara et al documented with MRI an increase in the retropalatal and retroglossal spaces with a Snore Guard or TheraSnore in place. Using the same sample of patients, Schwab et al147 found that the increase in cross-sectional area was related to a reduction in the thickness of the lateral pharyngeal walls. Miyazaki et al148 evaluated the TheraSnore in 11 OSA patients and found that 40% of patients had more than a 10% increase in their lowest oxygen saturation level and 70% demonstrated more than a 5% increase. The average RDI decreased from 49.5 to 32.0 and 60% of the patients reported an improvement in subjective symptoms. Tongue Retaining Device (TRD)
The TRD is a custom-made appliance with an anterior bulb that by means of negative pressure, holds the tongue forward during sleep. For those patients with blocked nasal passages, a modified TRD with lateral airway tubes to permit mouth breathing is also available. The FDA has granted marketing clearance for the TRD for the treatment of snoring. The TRD appliance is particularly useful in patients who have a large tongue. It is an effective alternative to a mandibular repositioner in patients with a compromised dentition or who are edentulous.33The TRD is the only appliance that has been studied in various body positions and in conjunction with other forms of therapy. Cartwright and Samelson 149evaluated 14 subjects and found a mean AI reduction from 54.4 to 22.7 after insertion of the TRD. In addition, improved sleep and significantly fewer and shorter apneic events were seen. The sleep architecture showed a change toward a more normal pattern with less light sleep and more 6-wave and more REM sleep immediately after the treatment began. The results seen were comparable with the rate reported for patients who had been treated either by tracheotomy or uvulopalatopharyngoplasty (UPPP). In a group of 16 male patients individuals with a substantial worsening of the AI while in the supine sleep position were more responsive to the TRD than those who were equally affected in both the lateral and supine position.
The AI in untreated subjects was twice as high while supine on their backs as it was in the side position. When obesity, age, and the position ratio were used in a discriminant function analysis, these three variables predicted TRD success (as defined by an Al < 6 or a 50% reduction in AI) correctly for 81% of the patients In a sample of 30 male patients. 65% tried on the TRD alone or in conjunction with other treatments were improved at the 1-year point. Samelson found that the TRD had an effect in 80% of subjects who had used it for 3 years or more. In another TRD report, a group of 12 subjects were treated with the TRD alone or in conjunction with some behavioral therapy such as sleep position training [60] or weight loss. A mean RDI reduction from37.0 to 17.3 was observed in this first group. In another group of with more severe apnea, the TRD was used in conjunction with a submucous resection of the septum or a UPPP. The TRD appears useful either alone or in conjunction with other treatments to improve patients with a wide range of apnea severity provided that the apnea is more severe in the supine position and the patient's weight is not greater than 50% above the ideal.33In another study150, a sample of 60 adult males with RDI values greater than 12.5who had two or more times the apnea rate during supine sleep in comparison to their lateral sleep rate were assigned to four treatment groups: TRD only, posture alarm, TRD plus posture alarm, and health habit instruction. Some 73% of the TRD group and 80% of the TRD plus posture alarm group improved. The 15subjects treated with the TRD alone had a reduction in mean RDI from 27.4 to11.4. Patency of the nasal airway and an initially low side index were the two factors significantly related to successful control of OSA with the TRD. For the15 subjects in the TRD plus posture alarm group, lower initial obesity and higher weight loss during treatment were the factors associated with best success. A mean RDI reduction from 30.7 to 7.9 was seen for the latter group. The effects of the TRD on baseline tongue muscle activity have been studied. Ono et al 151 found that the TRD has different effects on the awake genioglossus muscle activity in control subjects and OSA patients. In awake OSA patients, the TRD reduces genioglossus muscle activity and corrects the delayed timing of the muscle before an apneic period during sleep. The TRD may counteract fatigue in the tongue muscles and fluctuations in the activity of the genioglossus muscle. In addition, the TRD may provide a pneumatic splint to enlarge the upper airway similar to that seen with nCPAP.
OVERVIEW-
Oral appliance therapy for snoring, OSA, or both is simple, reversible, quiet, and cost effective and may be indicated in patients who are unable to tolerate nCPAP or who are poor surgical risks. Oral appliances are effective in varying degrees and appear to work because of an increase in airway space, the provision of a stable anterior position of the mandible, advancement of the tongue or soft palate, and possibly by a change in genioglossus muscle activity. The appliances should be used during sleep for life and must be comfortable for the patient. Ideally, they should have full occlusal coverage to prevent vertical changes to the dentition over time. The selection of patients suitable for oral appliance therapy must always be made by the attending physician. The dentist then selects the appropriate oral appliance. Documentation of the obstruction site is useful if such an assessment is available. Although traditional cephalometry can predict with some accuracy the volume of the tongue, soft palate, and nasopharynx, it is not a reliable indicator of oropharynx or hypopharynx size. If a small oropharynx is documented on the basis of CT or MRI evaluations, any appliance that could enlarge the airway by either advancing the tongue alone or advancing the mandible and the tongue together could be useful. If a disproportionately large tongue is seen or if the patient is edentulous or dentally compromised, a TRD could be effective. The TRD is even more effective if it is used in conjunction with behavioral modifications.
Mandibular repositioners all are effective in changing the three-dimensional size of the airway tube. Oral appliances have an effect on the tongue muscle either by advancing the mandible, holding the tongue forward, or altering the vertical dimension and thus affecting baseline tongue activity. Several contraindications for the use of oral appliances have been suggested but not all are applicable to any one appliance. Obviously, they should only be used for the treatment of obstructive and not central sleep apnea as quantified by overnight polysomnograms. If oral appliances simply rotate the mandible down and back while a predisposing constriction of the hypopharynx exists, the OSA may worsen. Oral appliances are not well tolerated by patients with arthritis, crepitus, or other significant temporomandibular joint symptoms; however, mild joint problems may be lessened by the forward jaw position. Sufficient healthy teeth to anchor the oral appliance are required for most appliances. Allergic and nasal obstructions may also be contraindications in selected patients. Finally, oral appliances can only be used in cooperative patients who are motivated to wear the appliance during sleep on a regular basis. Several questions require further study. How can one easily identify the obstruction site in a cost-effective way? Which patients are ideally suited for an oral appliance? Which appliance will be most effective in any one patient? What is the long-term compliance with these appliances? Are there any long-term deleterious effects on the temporomandibular joint or dentition? A long-term prospective study of the frequency and amount of occlusal changes is definitely required. Numerous simple solutions exist for the correction of minor tooth position changes, and long-term monitoring of these patients is definitely required. Patients demand alternatives to surgery and nCPAP, and the usefulness of oral appliances for the effective treatment of snoring or OSA is no longer in question. Three comparisons of oral appliances and nCPAP have been completed and a strong patient preference as well as good efficacy for oral appliances have been demonstrated. In addition, oral appliances have been found to be effective for patients who have not been treated successfully with uvulopalatopharyngoplasty. If the initial assessment is coordinated by the attending physician and good communication is established with the dentist involved, a significant number of subjects with snoring or mild-to-moderate OSA can be treated successfully with oral appliances.
To cure the material, direct the light source to both the buccal and the lingual surfaces to cure the material sufficiently before its separation from the articulator. Separate the prosthesis from the casts, place it in the Triad unit for final curing and finish it. Use the pressure-indicating paste clinically to reveal possible sources asneeded. Instruct the patient on how to insert the prosthesis properly and how to remove it. Provide counselling on procedures for care of the prosthesis at home.Complete dentures should be removed for a specific period during the day to void or minimize the adverse effects of continuous wear. At the follow-up evaluation, assess the quality of the patient’s sleep andcheck for the onset hypersomnolence and other related symptoms. The prosthesis should remain stable and retentive throughout the night, and the patient should befree of myofascial or temporomandibular joint symptoms. If discomfort develops, the prosthesis could be separated and the vertical dimension reduced.


No Any Replies to “OBSTRUCTIVE SLEEP APNEA”
Leave a Reply