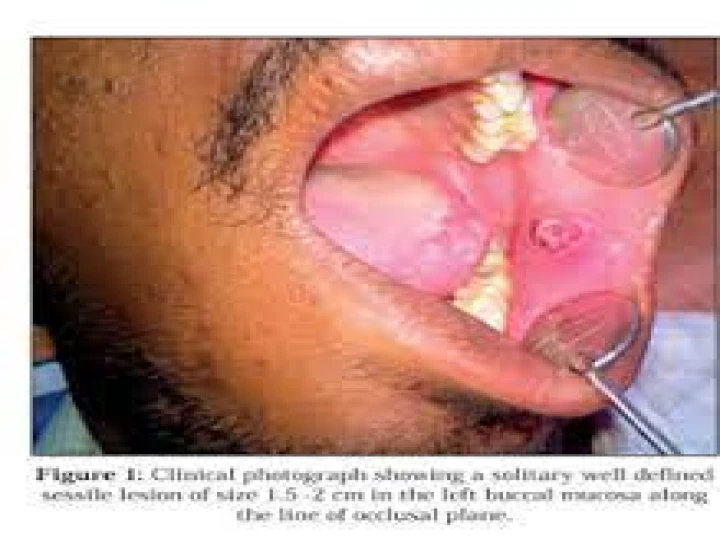
Schwannomas, also known as neurilemmomas, are benign tumors arising from Schwann cells, which are the cells responsible for the myelination of peripheral nerves. While relatively uncommon in the oral cavity, Schwannomas can occur anywhere along peripheral nerves, including the buccal mucosa. When located in the buccal mucosa, these tumors typically present as slow-growing, painless nodules that may or may not be associated with sensory disturbances.
The exact etiology of buccal mucosal Schwannomas is not well understood, although they are thought to arise from Schwann cells within the branches of the trigeminal nerve that innervate the oral mucosa. These tumors are usually solitary, encapsulated masses that can vary in size from a few millimeters to several centimeters in diameter. Although benign, Schwannomas can cause significant cosmetic concerns and functional impairment if they grow to a considerable size or impinge on adjacent structures.
Diagnosis of buccal mucosal Schwannomas often involves a combination of clinical examination and imaging studies. Clinically, they typically present as well-defined, round or ovoid masses that are firm and non-tender to palpation. Imaging modalities such as ultrasound, magnetic resonance imaging (MRI), or computed tomography (CT) scans may be used to further evaluate the size, location, and extent of the tumor, as well as its relationship to adjacent anatomical structures.
Histopathological examination remains the gold standard for definitive diagnosis of buccal mucosal Schwannomas. Microscopically, these tumors are characterized by the presence of spindle-shaped cells arranged in a palisading pattern around central acellular areas known as Verocay bodies. Immunohistochemical staining for S-100 protein, a marker for neural tissue, is typically positive, confirming the neural origin of the tumor.
Treatment of buccal mucosal Schwannomas usually involves surgical excision of the tumor with wide margins to prevent recurrence. In cases where the tumor is large or involves critical structures, such as major nerves or blood vessels, careful surgical planning may be required to preserve function while achieving complete tumor removal. Overall, the prognosis for buccal mucosal Schwannomas is excellent, with low rates of recurrence and minimal risk of malignant transformation. Early diagnosis and prompt intervention are essential for optimal outcomes in these cases.


No Any Replies to “SCHWANNOMA IN THE BUCCAL MUCOSA”
Leave a Reply